Model the Chances of Getting an Autoimmune Disease
Summary
Overview
Can genetic or environmental factors affect our chances of getting a certain disease? In this activity, your students will model how an existing predisposition can impact the probability of developing an autoimmune disease using dice and M&M's® candy!Learning Objectives
- Understand the factors that contribute to getting an autoimmune disease
- Explain why, in a given population, some people have an autoimmune disease, and some do not
- Apply the concepts of probability to model the likelihood of getting an autoimmune disease based on an existing predisposition
NGSS Alignment
This lesson helps students prepare for these Next Generation Science Standards Performance Expectations:- HS-LS3-3. Apply concepts of statistics and probability to explain the variation and distribution of expressed traits in a population.
|
Science & Engineering Practices
Developing and Using Models.
Develop and/or use a model (including mathematical and computational) to generate data to support explanations, predict phenomena, analyze systems, and/or solve problems.
Analyzing and Interpreting Data. Apply concepts of statistics and probability (including determining function fits to data, slope, intercept, and correlation coefficient for linear fits) to scientific and engineering questions and problems, using digital tools when feasible. Engaging in Argument from Evidence. Construct, use, and/or present an oral and written argument or counter-arguments based on data and evidence. |
Disciplinary Core Ideas
LS3.B: Variation of Traits. Environmental factors also affect expression of traits, and hence affect the probability of occurrences of traits in a population. Thus, the variation and distribution of traits observed depends on both genetic and environmental factors.
|
Crosscutting Concepts
Scale, Proportion, and Quantity.
Algebraic thinking is used to examine scientific data and predict the effect of a change in one variable on another (e.g., linear growth vs. exponential growth).
Systems and System Models. Models can be used to predict the behavior of a system, but these predictions have limited precision and reliability due to the assumptions and approximations inherent in models. |
Materials

Materials per class:
- Four desks
- Enough room to fit the whole class on each end of the desks (see Figure 2)
- Bowls or cups (8)
- M&M's candies (24 of each color: red, green, yellow, blue)
- Six-sided dice (6)
- Pencil or pen for each student
- Clear tape
Background Information for Teachers
This section contains a quick review for teachers of the science and concepts covered in this lesson.Our immune systems are made up of different cells and organs that normally defend us against pathogens (harmful microorganisms that can make us sick). The immune system goes through a process called the immune response to fight off a pathogen. Most of the work is done by white blood cells. There are several different types of white blood cells, including B cells and T cells; collectively, the different types of white blood cells are also called leukocytes. White blood cells must find the pathogen in the body, tell it apart from the body's regular cells, then make antibodies, which are tiny particles specifically designed to only attach, or bind, to the pathogen. Once bound to the pathogen, antibodies get help from white blood cells to destroy the pathogen.

An immune cell on the left and right compared when attached to both a self and non-self cell. Non-self cells will connect to non-self receptors, and self cells will connect to self receptors. However, self cells also have self antigens which attach to self antibodies.
Figure 1. Simplified diagram of the self/non-self recognition mechanism. In an autoimmune response, autoantibodies produced by immune cells bind to healthy body cells (self cells).
The process by which the immune system tells pathogens apart from own body cells is called self/nonself-recognition (Figure 1). If it fails, it can cause autoimmune disease or an infection. When the immune cells accidentally make an antibody that binds to its own body cells, it is called autoimmunity, or an autoimmune response, while the antibody is called an autoantibody. Autoimmunity is common and usually not serious, but if it is not stopped by the body, it can turn into an autoimmune disease, which is when the immune system chronically attacks healthy cells in the body. A person's genetics can make them predisposed, or more likely, to get an autoimmune disease. For example, some mutations within specific genes can cause an autoimmune disease. Environmental factors, such as where a person lives, what a person eats, and things that a person is exposed to, can also affect whether a person gets an autoimmune disease.
There are three checkpoints that the immune system follows in order to stop an autoimmune response from becoming an autoimmune disease (note that these steps are simplified).
- Checkpoint 1: Sometimes, white blood cells (specifically B cells, which are made in the bone marrow, or T cells, which are made in the thymus) are made that have autoimmunity, meaning their antibodies bind to healthy body cells. The body must destroy them before they escape from the bone marrow or thymus, or they can cause an autoimmune disease.
- Checkpoint 2: Right before an immune response is triggered to fight a pathogen, white blood cells (called regulatory T cells) make sure that other white blood cells are not accidentally attacking the body's own cells. They need to do their job correctly to prevent an autoimmune disease.
- Checkpoint 3: After a pathogen is destroyed in the body, white blood cells (specifically activated T cells and B cells) must destroy themselves (through a process called apoptosis) to stop the immune response, or it could lead to an autoimmune disease.
One common autoimmune disease that you could discuss with your students is diabetes mellitus type 1, more commonly known as type 1 diabetes. Type 1 diabetes is caused when the immune system attacks and destroys beta cells in the pancreas that normally make insulin. Before the effects of type 1 diabetes become visible, autoantibodies can be detected. Even if a person has autoantibodies, they are not guaranteed to get type 1 diabetes, but they do have an increased likelihood of developing diabetes over their lifetime. The more types of autoantibodies that are present, the greater the risk.
The incidence varies from about 0.013% of people in Northern Europe and the United States, to a high of 0.035% of people in Scandinavia and a low of 0.001% of people in Japan and China. There is a genetic component to this condition, but it is not completely genetic—environmental factors also matter. If it were completely genetic, then if one identical twin had diabetes, the other twin would also get it; however, medical records show that if one identical twin has diabetes, the other twin is only 30–50% likely to also get it. This, among other medical evidence, shows that both genetics and environment matter.
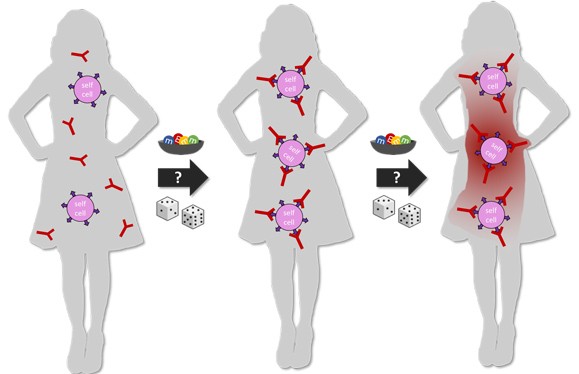
In this activity, students will use M&M's candies and a die to model the immune system and find out how a person's predisposition (genetics and other factors) affect whether they get an autoimmune disease or not.




