Stopping Superbugs!
Summary
Overview
If your doctor prescribes antibiotics, why do you have to take them for several days and not just once? Why do you need to finish taking them even if you feel better? If you do not follow the doctor's orders, you might contribute to the creation of antibiotic-resistant "superbugs"! In this lesson, your students will roll dice to model how bacteria respond to treatment by antibiotics, and find out what happens if treatment is stopped too early.
Learning Objectives
- Understand how natural selection leads to the predominance of certain traits in a bacterial population
- Correlate misuse of antibiotics with an increased probability of creating antibiotic-resistant bacteria
- Apply a model using probability to simulate how bacteria populations change in response to selective pressure
NGSS Alignment
This lesson helps students prepare for these Next Generation Science Standards Performance Expectations:- MS-LS4-4. Construct an explanation based on evidence that describes how genetic variations of traits in a population increase some individuals' probability of surviving and reproducing in a specific environment.
- MS-LS4-6. Use mathematical representations to support explanations of how natural selection may lead to increases and decreases of specific traits in populations over time.
|
Science & Engineering Practices
Developing and Using Models.
Develop and/or use a model to predict and/or describe phenomena.
Analyzing and Interpreting Data. Analyze and interpret data to provide evidence for phenomena. Apply concepts of statistics and probability (including mean, median, mode, and variability) to analyze and characterize data, using digital tools when feasible. Using Mathematics and Computational Thinking. Apply mathematical concepts and/or processes (e.g., ratio, rate, percent, basic operations, simple algebra) to scientific and engineering questions and problems. |
Disciplinary Core Ideas
LS4.B: Natural Selection.
Natural selection leads to the predominance of certain traits in a population, and the suppression of others.
LS4.C: Adaptation. Adaptation by natural selection acting over generations is one important process by which species change over time in response to changes in environmental conditions. Traits that support successful survival and reproduction in the new environment become more common; those that do not become less common. Thus, the distribution of traits in a population changes. |
Crosscutting Concepts
Cause and Effect.
Phenomena may have more than one cause, and some cause and effect relationships in systems can only be described using probability.
Systems and System Models. Models can be used to represent systems and their interactions—such as inputs, processes and outputs—and energy, matter, and information flows within systems. |
Materials

Materials per group of 4–6 students:
- Six-sided dice (100 total), in three different colors; available at Amazon.com:
- 70 of one color (purple in the picture)
- 25 of a second color (green in the picture)
- 5 of a third color (red in the picture)
- Pot, box, or sealable plastic bag that is large and sturdy enough to hold all 100 dice. If you use a metal pot, you may also want to use a lid to cut down on the noise of rolling the dice.
- Large, flat surface for pouring 100 dice onto
- Pencil or pen
Background Information for Teachers
This section contains a quick review for teachers of the science and concepts covered in this lesson.Bacteria are microscopic, single-celled organisms that are found everywhere. They are in the environment all around us, as well as inside and outside of our bodies. Most bacteria are harmless to humans, but some can cause serious illnesses. Any microorganism that makes us sick is called a pathogen. Antibiotics are the primary treatment for fighting bacterial infections. Before the discovery of the first antibiotic, penicillin, in 1928 by Alexander Fleming, people frequently died from minor wounds and infections (things we might think of as trivial injuries, like a scraped knee). Today, penicillin is estimated to have saved between 80–200 million lives.
However, many antibiotics have lost effectiveness because bacteria has become resistant to them over time, generating bacteria that are known as superbugs. Antibiotic resistance means that the bacteria have gained the ability to resist the effects of the drug that used to kill them. According to the Centers for Disease Control and Prevention (CDC) each year at least 2 million infections and 23,000 deaths are caused by antibiotic-resistant superbugs. Carbapenem-resistant Enterobacteriaceae (CRE) and methicillin-resistant Staphylococcus aureus (MRSA) are examples of these superbugs.
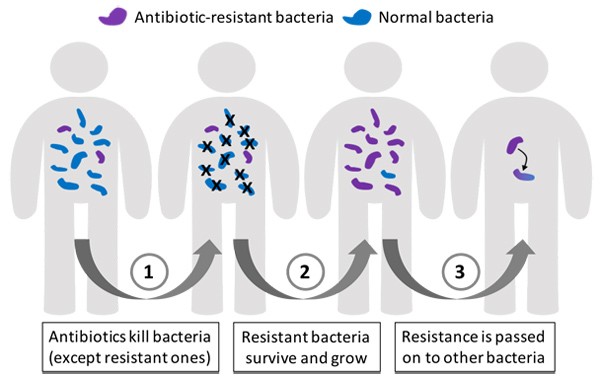
Bacteria that live in the human body are killed off with antibiotics except for a few resistant cells that survive. Any cell that survives a treatment of antibiotics will stay in the body and multiply creating more bacteria that are resistant.
Figure 1. Bacteria with antibiotic resistance survive an antibiotic treatment and pass their resistance on to other bacteria.
Antibiotic-resistant bacteria can be created in several ways. One way is through mutations of their genetic material which makes them less susceptible to the drug or allows the bacteria to deal with the antibiotic before it can do any harm. Another is the misuse of antibiotics. During an antibiotic treatment, the exposure to antibiotics creates a selective pressure on the bacteria which selects for the ones that are more resistant to the drug, as shown in Figure 1. The surviving bacteria are more likely to become antibiotic resistant and replace the bacteria that have been killed.
There are many ways for antibiotic-resistant bacteria to come about, including when a person:
- takes antibiotics they do not need (e.g., the person has a viral infection, which cannot be treated with antibiotics). In this case, all the bacteria in your body—the ones that can make you sick as well as the ones that help your body to function—get unnecessarily exposed to antibiotics and can develop resistances.
- improperly disposes of antibiotics (e.g., pours them down a drain and contaminates water systems). Antibiotics in our water are a great concern as all the bacteria that come in contact with these antibiotics can become antibiotic resistant and can pass their resistance to other bacteria in the environment.
- does not take the antibiotics long enough. This might happen because the patient forgets to take the antibiotics, feels better and stops taking them early, or dislikes the side effects of the antibiotics.
- takes the antibiotics for too long. In this case, all the pathogens will already be destroyed but other bacteria in our body will still be exposed to the antibiotics and can develop resistances.
All of these situations can result in selection for bacteria that are antibiotic resistant. This selection is based on the fact that not all bacteria are genetically the same. This difference in genetic traits make some bacteria more resistant to a certain antibiotic than others. This is also explains why it is not enough to take antibiotics just once when you are sick. As some bacteria have better strategies to resist the drug, they will survive one dose of antibiotics and it will take more doses to kill them. There is little research on what the perfect treatment time for antibiotics is, especially as it is also very dependent on the bacteria that is causing the illness. However, scientists agree that either taking antibiotics for too short a time, or too long a time increases the risk of creating antibiotic resistances.
In this lesson plan, students will simulate the selection for antibiotic-resistant bacteria by rolling dice to model how bacteria respond to treatment by antibiotics during a bacterial infection. In a bacterial infection, which can contain billions of bacteria, some bacteria will have a higher likelihood of surviving the treatment than others, based on their genetic traits. Thus, students will discover that if a patient stops taking antibiotics too early, it will influence the bacteria population and help the tougher, antibiotic-resistant bacteria to grow.